Chronic pancreatitis (CP) is a disease characterized by long standing pancreatic inflammation leading to irreversible fibrosis and structural changes in the pancreas. The prevalence of CP is estimated to be 125/100,000 population in India and is much more than the prevalence in the West. In India chronic pancreatitis forms an important pancreatic disease with varied presentations and treatment modalities.
Clinical Features of Chronic Pancreatitis: Unraveling the Symptoms and Complexity
Chronic pancreatitis is characterized by pancreatic atrophy, fibrosis, ductal strictures and distortion, calcifications, dysplasia, exocrine insufficiency and diabetes, and chronic pain. These various disease processes make treatment of chronic pancreatitis tricky with various treatment modalities that need to be tailored according to the disease course and situation.
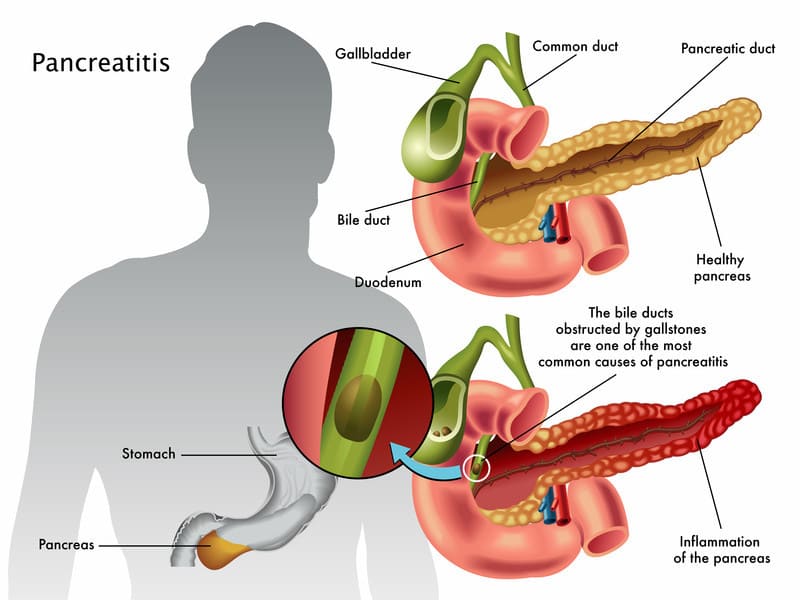
What are the most common causes of chronic pancreatitis?
Here following are most common causes of chronic pancreatitis in India
- Alcohol abuse is the most common aetiology of CP and is diagnosed in 42% to 77% of patients.
- Smoking is associated with chronic pancreatitis in a dose dependent fashion.
- Idiopathic CP is the second most common type and affects 28% to 80% of people with the condition.
- Several genetic mutations have been identified to be the cause of CP.
- Several genetic mutations have been identified to be the cause of CP.
- Other less common risk factors include increased calcium levels, increased triglyceride levels, auto- immune disorders (celiac disease, inflammatory bowel disease), and uncommon anatomic abnormalities in the pancreas such as an annular pancreas.
Diagnosing Chronic Pancreatitis: Exploring Diagnostic Techniques and Challenges
Contrast-Enhanced Computed Tomographic (CT) :
A contrast-enhanced computed tomographic (CT) scan is an initial diagnostic test and should be performed for all patients with suspicion of CP. Amylase and lipase are helpful for diagnosing acute pancreatitis but not CP. The presence of either calcifications, marked pancreatic ductal changes, or both of these findings on a CT scan establishes the diagnosis of CP. Magnetic resonance imaging(MRCP) may be used to look for ductal abnormalities.
Endoscopic Ultrasound :
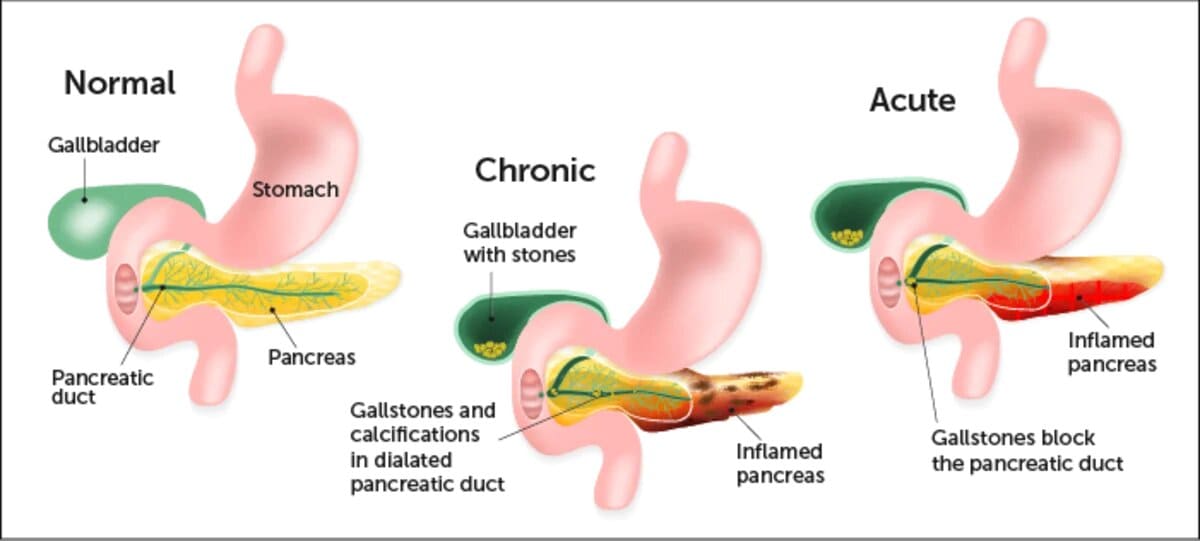
Endoscopic ultrasound is a very sensitive modality to diagnose chronic pancreatitis and may be required to diagnose chronic pancreatitis in early stages of the disease. Once chronic pancreatitis is diagnosed, a search for the cause of CP is looked for and corrected
Abdominal pain is present in more than 80% of patients with CP. Although classically reported as a dull pain localized to the epigastrium with radiation to the back that worsens after meals, the character, pattern, and severity of pain can vary. Other symptoms may include the onset of diabetes and symptoms of malabsorption like diarrhoea, steatorrhea(oily stools),weight loss and deficiency of fat soluble vitamins.
Managing Chronic Pancreatitis: Tailored Approaches for Treatment & Care
The treatment of chronic pancreatitis begins with medical management and moves on to invasive modalities like endoscopic therapies and finally surgery. Most therapies in chronic pancreatitis are directed at management of pain episodes in chronic pancreatitis.
Medical manageme supplementation and antioxidant therapy. Abstinence from alcohol and smoking forms the foundation for managing pain in CP. Medical therapy may not be successful in relieving pain in several patients and endoscopic treatnt of pain includes analgesics(pain killers),enzymement may be necessary. Not all patients may benefit from endoscopic therapy and choosing the right patient is necessary for best outcomes.
Endoscopic therapy includes clearance of obstructive stones from the pancreatic duct, dilatation of strictures and placement of pancreatic stent in the pancreatic duct to relieve obstruction. Endosonographic celiac plexus blockade may also be used to provide pain relief. Surgery may be helpful in certain candidates and provide lasting relief. Supplementation of pancreatic enzymes is necessary in patients with diarrhoea and steatorrhea. Management of diabetes forms an important part of managing CP. Screening for malignancy may be necessary in patients with long standing chronic pancreatitis or patients who experience a change in character of pain.
Treatment of a long standing disease like chronic pancreatitis with recurrent flares requires a multidisciplinary approach. Key treatment decisions need to be tailored individually, as no single treatment fits all and individualising treatment is the cornerstone of managing patients with CP.