Designation
Dr Sawan Bopanna
MD(Internal medicine,VMMC and Safadrajang Hospital), DM(Gastroenterology,AIIMS,New Delhi)
Consultant Gastroenterology,
Hepatology and Endoscopy
Senior Consultant
Action Gastrosciences and Liver Institute
Action Balaji Medical Institute
INTRODUCTION
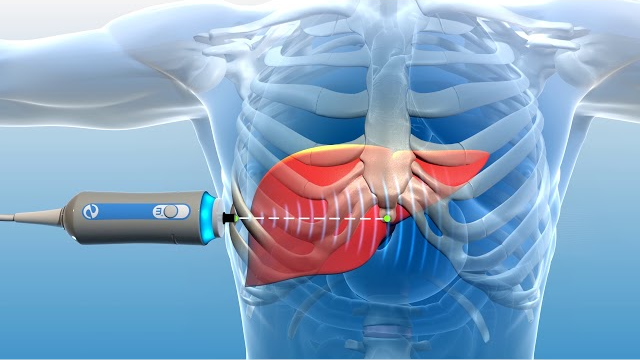
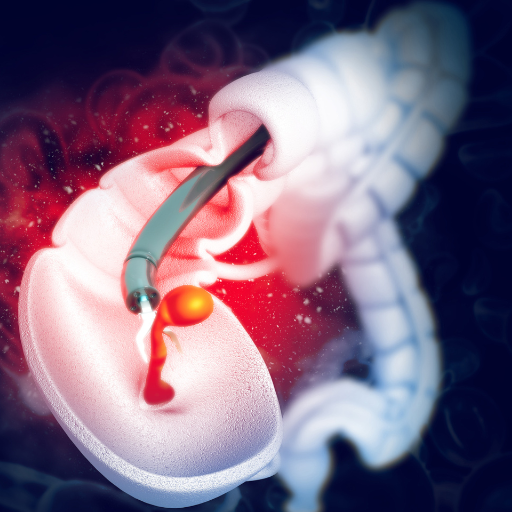
Dr Sawan Bopanna is a practicing consultant in Gastroenterology, Hepatology and Endoscopy in New Delhi. In a career spanning more than 13 years he has established himself as a doctor par excellence. "He previously served as a Senior Consultant at the Max Centre for Gastroenterology, Hepatology, and Endoscopy located at Max Superspeciality Hospital, Saket. Currently, he holds the position of Senior Consultant at the Department of Action Gastrosciences and Liver Institute within Action Balaji Medical Institute, Delhi." Being the best gastroenterologist in West Delhi, he has wide range of experience in treating complex diseases of the liver and gastrointestinal tract. His practice also includes performing advanced endoscopic procedures to cure gastrointestinal ailments. His strong forte is in performing endoscopic procedures like ERCP, endosonography and third space procedures.
Working in a centre with a wide range of evidence based treatment options for all liver and gastrointestinal diseases, patients may choose the most appropriate and cost effective treatment options all gastrointestinal problems. he known as a gastrology doctor in delhi, who ensure Ethical and reliable care with full disclosure to patients regarding advantages and disadvantages in his core priority
He received his training in prestigious medical institutions like Kasturba Medical College, Mangalore, Manipal Academy of Higher Education(MAHE), MD in Internal Medicine from VMMC and Safdarjung Hospital and DM in Gastroenterology from the All India Institute of Medical Sciences(AIIMS, New Delhi).
A keen academician with an active interest in research, he has many publications to his credit. He has contributed to various journals of national and international repute and published in these journals. He had been invited to faculty at various national conferences. He has presented various posters and papers at different conferences. He had made contributions to chapters and e-resources. He is one of the best gastroenterologists in west delhi and the best gastroenterologist in delhi NCR, provide one roof solution so to learn more about your condition book your consultation now
Read More
Explore Service
.png)








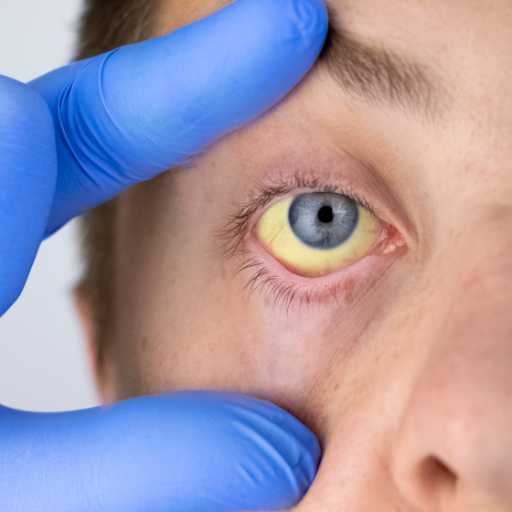



 >Services available at Gastro Liv Clinic
>Services available at Gastro Liv Clinic